Chuck DeBusk is Vice President; Performance & Process Improvement for UHS of Delaware, a subsidiary of Universal Health Services, Inc. - You can hear more about his experience in providing an excellent patient experience here.
The Goal: From a Provider Centric to Relationship Centric Patient Care
UHS operates 26 hospitals in 6 states and the District of Columbia. With these hospitals we operate with:
- 26 hospital based Emergency Departments
- 4 Freestanding Emergency Departments
- 1 million patient visits per year
- 3,100 visits per day.
With more ED beds plus ED-like care options (Free Standing EDs, Urgent Care, Minute Clinic, etc.), we have moved from a provider-centric model (where it was all about the hospital and the patient had to wait) to relationship-centric model.
In this model, what is important to the patient becomes critically important to the provider. Data tells us that patient’s value being kept informed, being seen by a physician quickly and getting through the process quickly. We decided to use the patient experience metric (gathered by Press Gainey) of “How well does the staff keep you informed of delays”. Our goal was to improve the patient experience by decreasing the length of stay while keeping patients better informed of delays.
WATCH THE FULL SESSION NOW: Improving Operational Throughput to Provide an Excellent Customer Experience
Through a series of projects, we decreased our Leaving without Being Seen (LWBS) rate from 1.9% in 2013 to 0.84% at the end of 2016. With the LWBS under better control in 2016 we turned our attention to throughput. Analysis of throughput revealed that the best opportunity to reduce wait time is in the ED Back-end process: patients that are being discharged and particularly for patients that are being admitted.
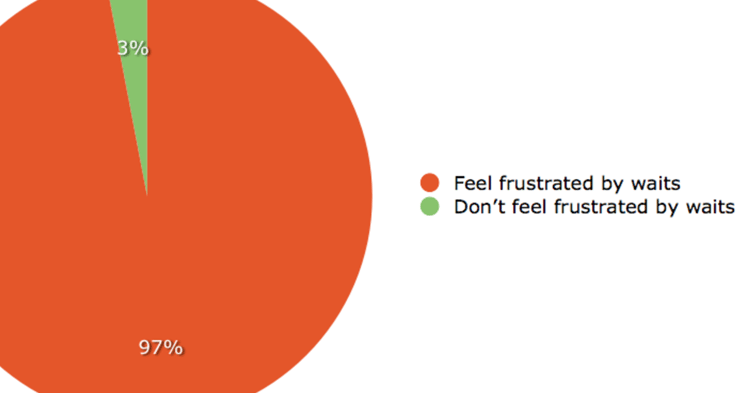
Reducing Patient Wait Times in the ED Back-end Process
Patients with a bed assignment were taking up to 90 minutes to leave the ED and be placed in an inpatient bed.
This occurred for a host of reasons, including:
- Admitting nurse not available for report
- Patient in bed not yet discharged (and on average that takes 4 hours)
- No one is available/willing to transport patient,
- Bed not clean because of miscommunication with EVS, etc.
Also, ED physicians continue to batch orders, including admission and discharge orders.
We began developing a proof of concept at Lakewood Ranch Medical Center. They have improved from a baseline of 27% meeting the goal of 60 minutes from Admission order to patient placement to 75% meeting the goal. At Lakewood Ranch we saw “How well did the staff keep you informed” improving from the 44th percentile to the 99th percentile. Length of stay for an admitted patient has decreased from 5.7 hours to 3.9.
Designing a process that moves the patient through the delivery of care in the Emergency Department especially focused on the time after care is rendered and the patient is medically ready to move to an inpatient bed until they are in that bed can reduce the variation felt by patients and reduce avoidable suffering. We've shown that by keeping patients informed, while driving a process that delivers more consistent results, we improve the patient experience on several levels.
We are continuing to deploy our improved practices throughout our Hospitals and Free Standing EDs. That will take 12 to 18 months.

About the Speaker
Chuck DeBusk is Vice President; Performance & Process Improvement for UHS of Delaware, a subsidiary of Universal Health Services, Inc. Chuck’s current role is to provide leadership to Operations and Clinical Process Improvement, Pharmacy, Surgery, Radiology and Laboratory. Chuck has over 30 years experience in healthcare and healthcare process improvement and is a Certified Lean Six Sigma Master Black Belt and a Registered Professional Engineer. He holds an MS in industrial engineering from the University of Tennessee and a BS in industrial engineering and operations research from Virginia Tech. He can be reached at Charles.debusk@uhsinc.com.
WATCH NOW: More Videos from BTOES17
Proqis Digital Virtual Conference Series
View our schedule of industry leading free to attend virtual conferences. Each a premier gathering of industry thought leaders and experts sharing key solutions to current challenges.
View Schedule of Events

.png)
-1.png)

















































-2.png)
-2.png)










%20(1)%20(1).png?width=1410&name=Add%20a%20heading%20(8)%20(1)%20(1).png)





.png?width=300&height=300&name=LINKEDIN%20AWARDS%20GRAPHIC%20(1).png)







-1.png?width=300&name=ATTENDEE%20-%20Proqis%20Digital%20Event%20Graphics%20(2)-1.png)
-1.png?width=300&name=ATTENDEE%20-%20Proqis%20Digital%20Event%20Graphics%20(1)-1.png)